| Research Article | ||
Open Vet. J.. 2025; 15(12): 6373-6378 Open Veterinary Journal, (2025), Vol. 15(12): 6373-6378 Research Article Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trialLucile S. L. Baía, Beni J. M. Chaúque and Régis A. Zanette*Graduate Program in Biological Sciences: Pharmacology and Therapeutics, Federal University of Rio Grande do Sul, Porto Alegre, Brazil *Corresponding Author: Régis A. Zanette. Laboratory of Experimentation in Drosophila, Basic Health Sciences Institute, Federal University of Rio Grande do Sul, Porto Alegre, Brazil. Email: regnitro [at] yahoo.com.br Submitted: 29/07/2025 Revised: 05/11/2025 Accepted: 17/11/2025 Published: 31/12/2025 © 2025 Open Veterinary Journal
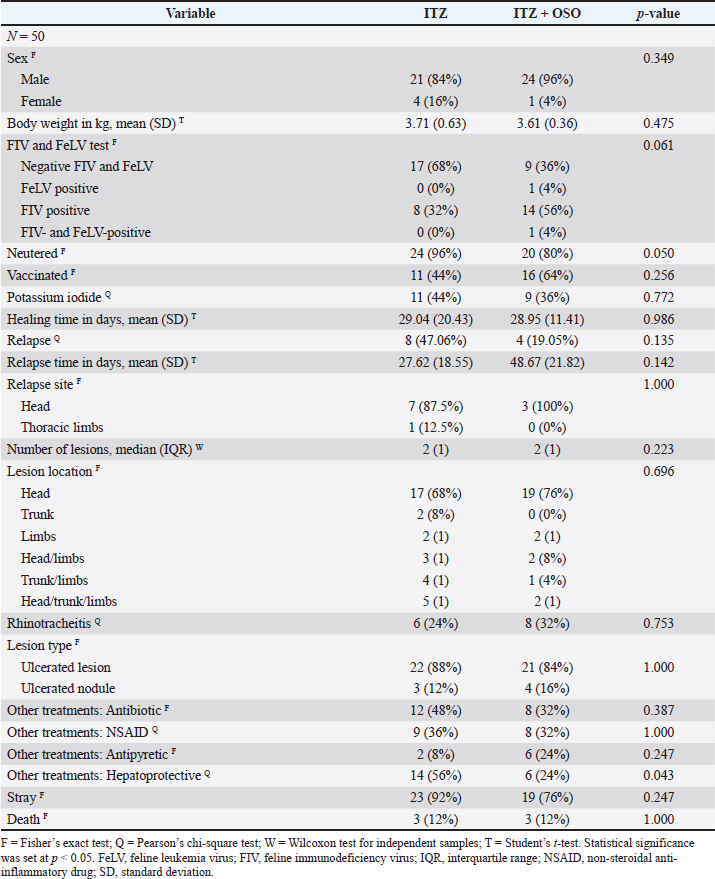
AbstractBackground: Feline sporotrichosis, primarily caused by Sporothrix brasiliensis, is a zoonotic fungal infection with limited therapeutic options. Aim: This study evaluated the efficacy of ozonized sunflower oil (OSO) as an adjunct to itraconazole (ITZ) in 50 cats with sporotrichosis. Methods: Animals were randomized into two groups: ITZ alone (100 mg/cat once daily, n=25) and ITZ plus topical OSO (700 meq/kg peroxide index, once daily, n=25). Primary outcomes (wound healing time) and secondary outcomes (relapse rate) were assessed over 120 days. Results: Although the healing times were similar (ITZ: 29.04 ± 20.43 days; ITZ + OSO: 28.95 ± 11.41 days; p=0.986), the ITZ + OSO group showed lower relapse rates (19.05% vs. 47.06%, p=0.135) and delayed recurrence (48.67 vs. 27.62 days, p=0.142). Notably, no relapses occurred in cats positive for feline immunodeficiency virus treated with ITZ + OSO (p=0.0027). Conclusion: The immunomodulatory and antifungal properties of OSO may enhance therapeutic outcomes, particularly in immunocompromised animals. Keywords: Sporotrichosis, Itraconazole, Ozonized sunflower oil, Integrative therapy, Feline. IntroductionSporotrichosis is a globally distributed zoonosis, predominantly found in tropical and subtropical regions due to favorable climatic conditions for its etiological agent (Rabello et al., 2022). The disease is caused by dimorphic fungi of the Sporothrix complex, with at least six pathogenic species, particularly Sporothrix schenckii and Sporothrix brasiliensis, the latter of which was identified in Brazil in 2007 and is now recognized as the most prevalent species in the country (Gremião et al., 2017; Da Rocha et al., 2018). Cats (Felis catus) serve as the primary transmission vectors, with infection typically occurring through traumatic inoculation via scratches or bites from infected animals (Gremião et al., 2017; Gremião et al., 2021). Fungal transmission may also result from contact with contaminated plants, soil, or decomposing organic matter, or less commonly through conidia inhalation (López Romero et al., 2011; Gremião et al., 2021). Self-inoculation through scratching or licking contributes to disease spread, with higher prevalence observed in intact male domestic shorthair cats due to their territorial behaviors (Pereira et al., 2014). These feline reservoirs significantly amplify environmental contamination, facilitating zoonotic transmission (Montenegro et al., 2014). Itraconazole (ITZ) remains the first-line treatment, although its utility is limited by hepatotoxicity, prolonged administration, and refractory cases (Da Rocha et al., 2018). Treatment success depends on multiple factors, including drug selection, dosing regimen, compliance, and fungal susceptibility (Nakasu et al., 2021). These limitations underscore the need to explore alternative therapies, particularly for patients exhibiting resistance to ITZ (Poester et al., 2019). Ozone (O3) therapy has emerged as a promising adjunctive approach for treating cancer. Ozone is an allotropic form of oxygen that acts as a potent oxidizing agent that disrupts microbial cell membranes by oxidizing amino acids and proteins. Against fungi, O3 specifically targets disulfide bonds in cell walls, penetrates the cytoplasm, and inhibits vital cellular functions while stimulating cellular and humoral immune responses (Ouf et al., 2016). Plant-derived ozonized oils represent a pharmaceutical approach to treating human and animal pathologies. Among these, ozonized sunflower oil (OSO) has demonstrated significant antifungal activity against Candida, Aspergillus, dermatophytes (Guimarães et al., 2020), and Sporothrix spp. (González, 2016). Therefore, this study evaluated the efficacy of OSO as a complementary therapy to ITZ for feline sporotrichosis. Materials and MethodsStudy location and experimental designInstitutionalized stray felines were selected from the Animal Welfare Center (CBEA) located in the city of Canoas, Rio Grande do Sul, Brazil. The CBEA is a municipal public institution responsible for sheltering, housing, sterilizing, and eventually adopting street animals and those subjected to domestic abuse. The research was conducted between August 2024 and April 2025 through an open clinical trial involving 50 animals randomly allocated in a 1:1 ratio into two groups of 25 animals each, with no preference for age, weight, or sex. The following inclusion (a) and exclusion (b) criteria were applied: a) wounds and or ulcerated nodules contaminated with Sporothrix spp., varying in size and anatomical distribution; b) animals with a low body condition score, feral behavior, and negative fungal culture and isolation. DiagnosisThe diagnosis was confirmed by collecting lesion samples with a sterile swab in a specific transport medium, followed by fungal isolation onto chloramphenicol-supplemented Sabouraud Dextrose Agar plates. Plates were incubated at 25°C–29°C for 15 days. A colony fragment was transferred onto yeast extract peptone dextrose agar plates and incubated at 37°C for 7 days to induce the dimorphic transition from mycelial to yeast form, confirming the characteristic fungal dimorphism. Fungal structures were microscopically identified based on morphological characteristics. Therapeutic protocolThe ITZ group received compounded ITZ, provided by the institution, orally, at a dose of 100 mg cat once daily (Gremião et al., 2021). The ITZ oil group received conventional ITZ therapy combined with topical OSO, once daily, with a peroxide index of 700 meq kg, commercially obtained from Ozone Health São Paulo, Brazil. Before oil application, the wounds were cleaned with 0.9% saline solution. The veterinarian in charge of the CBEA sporotrichosis isolation unit performed all therapeutic procedures daily in the morning, following personal protective equipment (PPE) protocols (gloves, gowns, goggles, and masks). Weekly lesion monitoring was conducted through visual assessment and photographic documentation (with date and time). The following outcomes were analyzed: (i) time to ulcerative lesion resolution (primary outcome) and (ii) time to recurrence (secondary outcome). The observation window for these outcomes was set at 120 days per animal per group. Data analysisThe sample size was calculated based on CBEA epidemiological reports from August 2023 to April 2024 in Canoas, RS, Brazil. The methodological approach included descriptive and inferential analyses, with the selection of parametric and non-parametric tests depending on the nature and distribution of the variables. The normality assumption for continuous variables (body weight, healing time, and time to relapse) was evaluated using the Shapiro–Wilk test. Since all variables exhibited normal distribution (p > 0.05), comparisons between groups were conducted using Student’s t-test for independent samples. For the number of wounds, which showed asymmetric distribution (p < 0.001), the Wilcoxon test (non-parametric) was used. Categorical variables—sex, immunodeficiency virus (FIV) and feline leukemia virus (FeLV) status, and recurrence—were analyzed using Fisher’s exact test or Pearson’s chi-square test. A 95% significance level (p < 0.05) was adopted. Ethical approvalThe Animal Ethics Committee (CEUA/UFRGS) approved the project under protocol number 45947. Date: 07/26/2024. All experiments were conducted in accordance with Brazilian Law N. 11,794–2008 (Procedures for the Scientific Use of Animals) and the Council for International Organizations of Medical Sciences’ international guidelines for biomedical research involving animals. The research followed ethical standards, ensuring the minimization of animal discomfort and pain. The use of PPE and compliance with "Cat Friendly" practices, following the American Association of Feline Practitioners Guidelines, demonstrates a commitment to the welfare of the felines involved in the study. ResultsTable 1 presents the comparative outcomes of the two therapeutic protocols for feline sporotrichosis, including clinical, demographic, and endpoint variables (healing time, relapse, and mortality). The sample consisted of 50 felines that were equally distributed between the ITZ group (n=25) and the ITZ + OSO group (n=25). Table 1. Comparison between therapeutic protocols using itraconazole (ITZ) versus ITZ + ozonized sunflower oil (OSO) in cats with sporotrichosis: a meta-analysis.
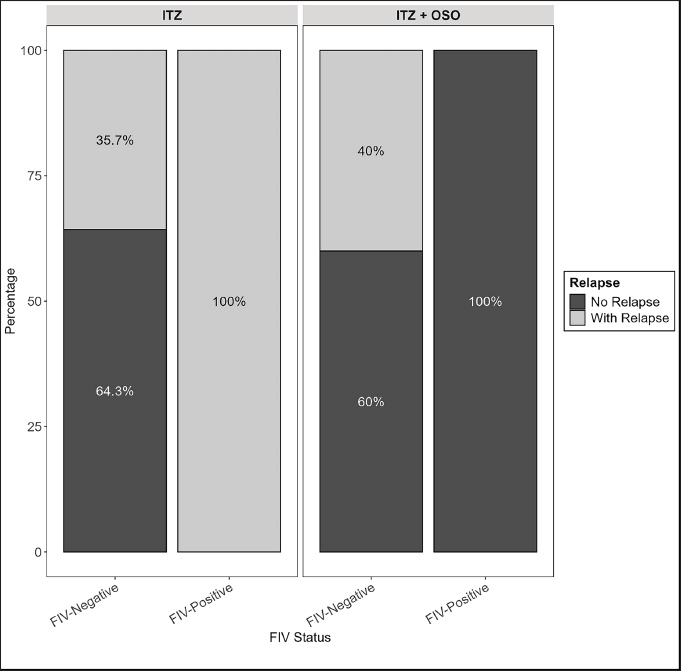
Despite the lack of statistical significance (p=0.135), a clinically meaningful difference emerged: 47.06% of animals in the ITZ group experienced relapse, compared to only 19.05% in the ITZ + OSO group. Notably, among animals with relapse, the time to lesion reappearance was longer in the ITZ + OSO group than in the ITZ + OSO group (p=0.142). Lesions located exclusively on the head were associated with a lower relapse rate, whereas wounds involving multiple regions, such as the limbs, trunk, or their combinations, were associated with a higher likelihood of relapse. Although healing time did not differ between the groups (p=0.986), the ITZ + OSO group exhibited clinically relevant trends, including a lower relapse rate and a longer time to relapse. Figure 1 explores the interaction between the FIV status and relapse. All FIV-positive animals in the ITZ group experienced relapse, whereas no relapse was observed among FIV-positive animals in the ITZ + OSO group (p=0.0027). Relapse rates were comparable between groups among FIV-negative individuals, reinforcing that the ITZ + OSO protocol may be more effective in immunocompromised patients.
Fig. 1. Distribution of relapse and feline immunodeficiency virus (FIV) status in felines with sporotrichosis treated with ITZ or ITZ + ozonized sunflower oil (OSO). Fisher´s Exact Test (FIV+): p=0.0027. Hepatoprotective agent use was significantly more frequent in the ITZ group (p=0.043). No significant differences were observed in the use of antibiotics, non-steroidal anti-inflammatory drugs, or antipyretics. The mortality rates were identical in both groups. DiscussionAlthough the average healing time did not differ significantly between the groups, the combination of OSO with ITZ showed favorable trends in reducing recurrences, corroborating previous findings on the antifungal and immunomodulatory effects of ozone therapy (Ouf et al., 2016; Rodrigues et al., 2020). The practical implications of these results are significant, as they support strategies aimed at preventing new infections—an essential component in the effective management of this comorbidity. For example, for FIV+ felines, OSO appears to have contributed to the absence of relapses. Feline sporotrichosis represents a significant therapeutic challenge in veterinary medicine, particularly in endemic regions (Gremião et al., 2021; Siqueira, 2021). Ozone therapy has emerged as a growing complementary treatment method in this field, as it provides various benefits for animals when used alongside conventional treatment. Calheiros et al. (2023) found that the combination of ITZ with ozone therapy applied via "bagging" was effective in treating a feline with sporotrichosis. The sessions were conducted weekly, with the first two performed at a high concentration (52 μg ml) and the subsequent sessions at a lower concentration (20 μg ml). This alternative therapy was employed after no clinical improvement was observed with ITZ-based treatment, along with debridement and wound cleaning. Siqueira (2021) also observed positive results from the use of ITZ combined with ozone therapy as an adjuvant treatment in a feline with sporotrichosis. The antifungal was administered at a dose of 10 mg kg, PO, SID, for 6 months, while ozone therapy included rectal insufflation, subcutaneous O3 applications in the cervical region, and daily OSO applications. This approach led to complete regression of lesions and clinical improvement in a shorter time than expected compared with conventional ITZ treatment. From a technical and therapeutic perspective, ozonized oil proved superior not only in preventing recurrences but also in prolonging the time until lesion recurrence (48.67 days in the ITZ + OSO group vs. 27.62 days in the ITZ group). Conventional ITZ treatment, although effective in many cases, faces several obstacles, particularly early relapse, hepatic toxicity, and fungal resistance development (Lloret et al., 2013). Thus, the combined approach serves as an alternative to mitigate these risks. For example, Siqueira (2021) reported that this therapeutic combination reduced common adverse effects of prolonged therapies, such as gastroesophageal reflux, vomiting, and hepatotoxicity. The integrative use of OSO is a promising alternative, opening new perspectives for disease management, particularly in high-risk patients. The efficacy of OSO can be attributed to its multifactorial action, combining direct antimicrobial effects and improved tissue oxygenation (Travagli et al., 2010). O3 reacts with unsaturated fatty acids in the oil, forming ozonides and peroxides, which are potent oxidizing agents. These reactive oxygen species damage the Sporothrix cell wall, causing structural rupture and fungal death (Ouf et al., 2016). Unlike ITZ, which inhibits ergosterol synthesis, the mechanism of OSO is nonspecific, based on indiscriminate and irreversible oxidation, potentially reducing the likelihood of fungal resistance. Chronic immunosuppression in FIV+ cats compromises the response to conventional treatment. Coinfection with retrovirus and Sporothrix leads to significant immune imbalances, favoring an immunosuppressive profile with elevated IL-10 levels, which may hinder the activation of a Th1 response—essential for combating sporotrichosis (Miranda et al., 2018). OSO stimulates the production of proinflammatory cytokines, including interferon-γ and interleukin-2, thereby enhancing Th1-mediated immune responses. Additionally, evidence suggests that O3 activates macrophages and increases the expression of transcription factors, such as nuclear factor erythroid-2 related factor 2, which regulate cellular antioxidant responses and protect tissues against excessive oxidative damage (Ouf et al., 2016). Chronic lesions in cats with sporotrichosis often exhibit poor oxygenation and persistent inflammation. The ozonides in OSO improve tissue perfusion by promoting angiogenesis and collagen synthesis through controlled oxygen release. Despite these findings, this study has some limitations. The relatively small sample size (50 felines) may hinder the generalizability of the results. Future studies with larger cohorts and standardized protocols are needed to confirm these conclusions and explore the mechanisms underlying the beneficial effects of OSO. Conducting the study with a larger number of animals under varying clinical conditions could provide more robust and conclusive data. Standardizing protocols defining optimal O3 concentrations, application frequency, and incorporating molecular studies assessing immune markers (e.g., cytokine profiles) could further enhance the findings. In addition, patient follow-up was limited to 120 days per group, and the lack of long-term monitoring may obscure potential late recurrences or adverse effects. Undocumented pre-existing health conditions among the animals may also have influenced the observed efficacy of this study. From an economic standpoint, ozonized oil offers substantial advantages, as its production is low-cost, using accessible raw materials. The reduced need for adjuvant treatments (e.g., antibiotics) and lower recurrence rates position OSO as a more cost-effective long-term option, particularly in resource-limited regions or for low-income owners. ConclusionIn summary, OSO shows promise as a fair and feasible adjunct therapy for cutaneous sporotrichosis in cats, particularly in the context of FIV coinfection. However, additional studies are needed to strengthen these observations. Its multidimensional benefits—from therapeutic efficacy to accessibility and sustainability—underscore its potential to redefine chronic wound management in this population. Continued research, with regular and careful monitoring, is essential to validate the safety and efficacy of OSO. AcknowledgmentsThe authors would like to thank the staff of the Centro de Bem-Estar Animal, especially Marina Diogo da Silva and Tatiane Berto, for their invaluable assistance in the care of the animals used in this study. Conflict of interestThe authors declare no conflict of interest. FundingThe Brazilian National Council for Scientific and Technological Development (CNPq) provided a scholarship to R. A. Z. Authors’ contributionsThe study was conceptualized by LSLB and RAZ. LSLB performed fieldwork, data retrieval, and analysis. LSLB and BJMC drafted the manuscript. RAZ revised and edited the manuscript. All authors have approved the final version of the manuscript. Data availabilityThe data that support the findings of this study are not openly available due to sensitivity reasons and are available from the corresponding author upon reasonable request. ReferencesCalheiros, A.S., Calheiros, L.G.M., Carnaúba, R.T.M.S., Caldas Júnior, N.M., Souza Filho, N.C. and Lima, A.D.S. 2023. Associação da ozonioterapia com itraconazol para tratamento das lesões de esporotricose felina: relato de caso. Vet. Zootec. 30(1), 1–6. Da Rocha, R.F.D.B., Schubach, T.M.P., Pereira, S.A., Dos Reis, E.G., Carvalho, B.W. and Gremião, I.D.F. 2018. Refractory feline sporotrichosis treated with itraconazole combined with potassium iodide. J. Small Anim. Pract. 59, 720–721. González K. 2016. Actividad antifúngica in vitro de aceite de girasol ozonizado en hongos causales de micosis superficiales. Undergraduate thesis, Especialización en Micología Médica, República Bolivariana de Venezuela. Gremião, I.D.F., Martins Da Silva Da Rocha, E., Montenegro, H., Carneiro, A.J.B., Xavier, M.O., De Farias, M.R., Monti, F., Mansho, W., De Macedo Assunção Pereira, R.H., Pereira, S.A. and Lopes-Bezerra, L.M. 2021. Guideline for the management of feline sporotrichosis caused by Sporothrix brasiliensis and literature revision. Braz. J. Microbiol. 52, 107–124. Gremião, I.D.F., Miranda, L.H.M., Reis, E.G., Rodrigues, A.M. and Pereira, S.A. 2017. Zoonotic epidemic of sporotrichosis: cat to human transmission. PLos Pathog. 13, e1006077. Guimarães, N.M., Oliveira, I.F. and Kozusny-Andreani, D.I. 2020. Eficácia de óleos vegetais in natura e ozonizados no controle de Sporothrix schenckii. Int. J. Dev. Res. 10, 41970–41974. Lloret, A., Hartmann, K., Pennisi, M.G., Ferrer, L., Addie, D., Belák, S., Boucraut-Baralon, C., Burny, A., Canuti, M., Carvelli, A., Egberink, H., Fontbonne, A., Fossum, S., Gruffydd-Jones, T., Hosie, M.J., Hoskins, J., Lappin, M., Marsilio, F., Reinacher, M., Thiry, E., Truyen, U. and Addie, D.D. 2013. Sporotrichosis in cats: aBCD guidelines on prevention and management. J. Feline. Med. Surg. 15, 619–623. López-Romero, E., Reyes-Montes, M.D.R., Pérez-Torres, A., Ruiz-Baca, E., Villagómez-Castro, J.C., Mora-Montes, H.M., Flores-Carreón, A. and Toriello, C. 2011. Sporothrix schenckii complex and sporotrichosis, an emerging health problem. Future. Microbiol. 6, 85–102. Miranda, L.H.M.D., Meli, M., Conceição-Silva, F., Novacco, M., Menezes, R.C., Pereira, S.A., Sugiarto, S., Reis, E.G.D., Gremião, I.D.F. and Hofmann-Lehmann, R. 2018. Co-infection with feline retrovirus is related to changes in immunological parameters of cats with sporotrichosis. PLos One. 13, 207644. Montenegro, H., Rodrigues, A.M., Dias, M.A.G., Da Silva, E.A., Bernardi, F. and De Camargo, Z.P. 2014. Feline sporotrichosis due to Sporothrix brasiliensis: an emerging animal infection in São Paulo, Brazil. BMC Vet. Res. 10, 1–11. Nakasu, C.C.T., Waller, S.B., Ripoll, M.K., Ferreira, M.R.A., Conceição, F.R., Gomes, A.D.R., Osório, L.D.G., De Faria, R.O. and Cleff, M.B. 2021. Feline sporotrichosis: a case series of itraconazole-resistant Sporothrix brasiliensis infection. Braz. J. Microbiol. 52, 163–171. Ouf, S.A., Moussa, T.A., Abd-Elmegeed, A.M. and Eltahlawy, S.R. 2016. Anti-fungal potential of ozone against some dermatophytes. Braz. J. Microbiol. 47, 697–702. Pereira, S.A., Gremião, I.D.F., Kitada, A.A.B., Boechat, J.S., Viana, P.G. and Schubach, T.M.P. 2014. The epidemiological scenario of feline sporotrichosis in Rio de Janeiro, State of Rio de Janeiro, Brazil. Rev. Soc. Bras. Med. Trop. 47, 392–393. Poester, V.R., Mattei, A.S., Mendes, J.F., Klafke, G.B., Ramis, I.B., Sanchotene, K.O. and Xavier, M.O. 2019. Antifungal activity of diphenyl diselenide alone and in combination with itraconazole against Sporothrix brasiliensis. Med. Mycol. 57, 328–331. Rabello, V.B.S., Almeida, M.A., Bernardes-Engemann, A.R., Almeida-Paes, R., De Macedo, P.M. and Zancopé-Oliveira, R.M. 2022. The historical burden of sporotrichosis in Brazil: a systematic review of cases reported from 1907 to 2020. Braz. J. Microbiol. 53, 231–244. Rodrigues, A.M., Della Terra, P.P., Gremião, I.D., Pereira, S.A., Orofino-Costa, R. and De Camargo, Z.P. 2020. The threat of emerging and re-emerging pathogenic Sporothrix species. Mycopathologia 185, 813–842. Siqueira, R.M. 2021. Efecto clínico de la ozonoterapia como tratamiento complementario en un gato con esporotricosis. Reporte de caso. Ozone Ther. Glob. J. 11, 151–161. Travagli, V., Zanardi, I., Valacchi, G. and Bocci, V. 2010. Ozone and ozonated oils in skin diseases: a review. Mediators. Inflamm. 2010, 610418. | ||
| How to Cite this Article |
| Pubmed Style Baía LSL, Chaúque BJM, Zanette RA. Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Vet. J.. 2025; 15(12): 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 Web Style Baía LSL, Chaúque BJM, Zanette RA. Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. https://www.openveterinaryjournal.com/?mno=274152 [Access: January 25, 2026]. doi:10.5455/OVJ.2025.v15.i12.21 AMA (American Medical Association) Style Baía LSL, Chaúque BJM, Zanette RA. Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Vet. J.. 2025; 15(12): 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 Vancouver/ICMJE Style Baía LSL, Chaúque BJM, Zanette RA. Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Vet. J.. (2025), [cited January 25, 2026]; 15(12): 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 Harvard Style Baía, L. S. L., Chaúque, . B. J. M. & Zanette, . R. A. (2025) Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Vet. J., 15 (12), 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 Turabian Style Baía, Lucile S. L., Beni J. M. Chaúque, and Régis A. Zanette. 2025. Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Veterinary Journal, 15 (12), 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 Chicago Style Baía, Lucile S. L., Beni J. M. Chaúque, and Régis A. Zanette. "Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial." Open Veterinary Journal 15 (2025), 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 MLA (The Modern Language Association) Style Baía, Lucile S. L., Beni J. M. Chaúque, and Régis A. Zanette. "Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial." Open Veterinary Journal 15.12 (2025), 6373-6378. Print. doi:10.5455/OVJ.2025.v15.i12.21 APA (American Psychological Association) Style Baía, L. S. L., Chaúque, . B. J. M. & Zanette, . R. A. (2025) Ozonized sunflower oil as an integrative therapy for feline sporotrichosis: a randomized clinical trial. Open Veterinary Journal, 15 (12), 6373-6378. doi:10.5455/OVJ.2025.v15.i12.21 |